Neural tube defects (NTDs) are one of the most significant congenital disorders, impacting thousands of families worldwide. These birth defects occur when the neural tube, which forms the brain and spinal cord during the initial stages of embryonic development, does not close properly. Within the first month of pregnancy—often before a woman realizes she’s pregnant—this critical process takes place. NTDs include conditions like spina bifida and anencephaly, which can lead to severe disabilities or are incompatible with life. Understanding the causes, preventive measures, and management options for NTDs is essential for reducing their occurrence and improving outcomes for affected families.
What Causes Neural Tube Defects? Genetic and Environmental Risk Factors
Neural tube defects arise from a combination of genetic and environmental factors. Genetic predisposition plays a substantial role, with studies estimating that 70% of NTD cases are influenced by inherited genetic factors. Mutations in genes responsible for folate metabolism, such as the methylenetetrahydrofolate reductase (MTHFR) gene, are particularly significant. These mutations impair the body’s ability to process folate, a vitamin essential for cell division and neural tube formation, thereby increasing susceptibility to defects.
In families with a history of NTDs, the risk of recurrence is significantly higher. For example, couples who have had one child with an NTD face a 2-4% risk of recurrence in subsequent pregnancies. This risk escalates to approximately 10% if two or more children are affected. These figures underscore the importance of genetic counseling for families with a history of NTDs.
Environmental factors also contribute to the development of NTDs. Maternal diabetes, exposure to certain medications like valproic acid (commonly used for epilepsy), and toxins such as fumonisin (found in contaminated maize) are all associated with increased risk. Additionally, behaviors like frequent use of hot tubs or saunas during early pregnancy and unmanaged maternal fevers can negatively impact fetal neural development.
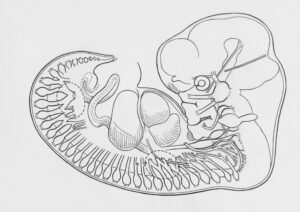
Severe Neural Tube Defect: Understanding Craniorachischisis
Craniorachischisis is one of the most severe and rare forms of neural tube defects. This condition results from the complete failure of the neural tube to close, leading to both anencephaly and spina bifida. Fetuses affected by craniorachischisis often exhibit profound malformations, including the absence of cranial bones and brain tissue. Unfortunately, this condition is incompatible with life, and most affected fetuses do not survive to term or live beyond the neonatal period.
Medical professionals rely on prenatal imaging, such as ultrasounds, to diagnose craniorachischisis. Key diagnostic features include the absence of cranial bones, an incomplete brain, and a U-shaped vertebral column in axial scans. In coronal scans, the wide separation of spinous processes confirms the diagnosis.
Although craniorachischisis is exceedingly rare, its study provides invaluable insights into the genetic and environmental interactions that underlie neural tube defects. Researchers continue to investigate its causes to better understand the mechanisms of neural tube closure.
Recurrence of Neural Tube Defects in Pregnancy: What You Need to Know
Families who experience an NTD-affected pregnancy often face heightened anxiety about recurrence. With a 2-4% recurrence rate following one affected pregnancy and a risk as high as 10% with two affected children, these families require specialized care and support. Early intervention, genetic counseling, and proactive prenatal care are essential for mitigating these risks.
For example, in one reported case, a woman with a history of anencephaly in a previous pregnancy experienced a recurrence of NTD in her current pregnancy. Contributing factors included inadequate prenatal care and delayed folic acid supplementation. Genetic testing revealed a predisposition to NTDs, highlighting the critical importance of preventive measures.
Couples with a history of NTDs should consult healthcare professionals to develop a comprehensive preconception and prenatal care plan. This includes addressing risk factors and ensuring early and adequate folic acid intake.
Folic Acid: The Key to Preventing Neural Tube Defects
Folic acid is a well-established preventive measure for neural tube defects. This synthetic form of folate, a B-vitamin, is vital for DNA synthesis, repair, and cell division—especially during the critical early stages of pregnancy when the neural tube forms. Research indicates that adequate folic acid intake can prevent up to 70% of neural tube defects, making it one of the most effective interventions available.
Health authorities recommend that all women of childbearing age consume 400 micrograms (mcg) of folic acid daily, as neural tube closure occurs within the first 28 days of pregnancy. For women with a history of NTDs or other high-risk factors, a higher dose of 5 milligrams (mg) per day is recommended. This supplementation should begin at least three months before conception and continue through the first trimester.
In one case, a patient who began folic acid supplementation late in her pregnancy—after the first trimester—experienced a recurrence of an NTD. This underscores the importance of early initiation of folic acid and timely prenatal care. Public health campaigns have been successful in raising awareness about folic acid, but more efforts are needed to address barriers such as socioeconomic disparities and lack of access to healthcare.

Obstetric Management of Severe Neural Tube Defects
When severe neural tube defects like craniorachischisis are diagnosed, obstetric management focuses on compassionate care and minimizing risks to the mother. In many cases, termination of the pregnancy is considered due to the incompatibility of such defects with life.
Medical professionals use prostaglandins to induce labor for pregnancy termination in these cases. Vaginal delivery is the preferred method, as it reduces surgical risks and provides a safer option for the mother. In addition to physical considerations, healthcare providers must navigate ethical and emotional challenges, ensuring that patients receive comprehensive counseling and support.
Early and accurate diagnosis through prenatal ultrasound and genetic testing is essential for managing pregnancies affected by severe NTDs. These tools allow families to make informed decisions and plan for appropriate care.
Conclusion
Neural tube defects remain a significant public health issue, despite advances in prevention and management. Understanding the multifactorial causes of NTDs, including genetic predispositions and environmental risk factors, is crucial for developing effective interventions. Folic acid supplementation, when initiated early, is a powerful tool in reducing the prevalence of these conditions.
Severe cases of NTDs, such as craniorachischisis, highlight the need for compassionate and personalized care. Families facing these challenges benefit from comprehensive support systems, including genetic counseling and tailored prenatal care.
By raising awareness, improving access to healthcare, and addressing disparities, we can continue to reduce the burden of neural tube defects and improve outcomes for affected families. Through collective efforts, a future where NTDs are a rarity is within reach.
Reference
- Causes and Risk Factors of Neural Tube Defects Centers for Disease Control and Prevention. (n.d.). Neural tube defects. Retrieved from https://www.cdc.gov/birthdefects/about/neural-tube-defects.html
- Craniorachisis and Clinical Signs Radiopaedia. (n.d.). Craniorachischisis. Retrieved from https://radiopaedia.org/articles/craniorachischisis
- Relationship Previous Pregnancy and Anencephaly in the Current Pregnancy De Gruyter. (n.d.). Anencephaly: Recurrence and prevention strategies. Retrieved from https://www.degruyter.com/document/doi/10.1515/jpm-2017-0363/html
- Justification for Folic Acid Use in the New Pregnancy UpToDate. (n.d.). Preconception and prenatal folic acid supplementation. Retrieved from https://www.uptodate.com/contents/preconception-and-prenatal-folic-acid-supplementation
- Obstetric Behavior of the Medical Staff American College of Obstetricians and Gynecologists. (2017). Behavior that undermines a culture of safety. Retrieved from https://www.acog.org/clinical/clinical-guidance/committee-opinion/articles/2017/01/behavior-that-undermines-a-culture-of-safet

Good
Very good
Yeniköy su kaçak tespiti Güler yüzlü ekip sayesinde tüm endişelerim ortadan kalktı.